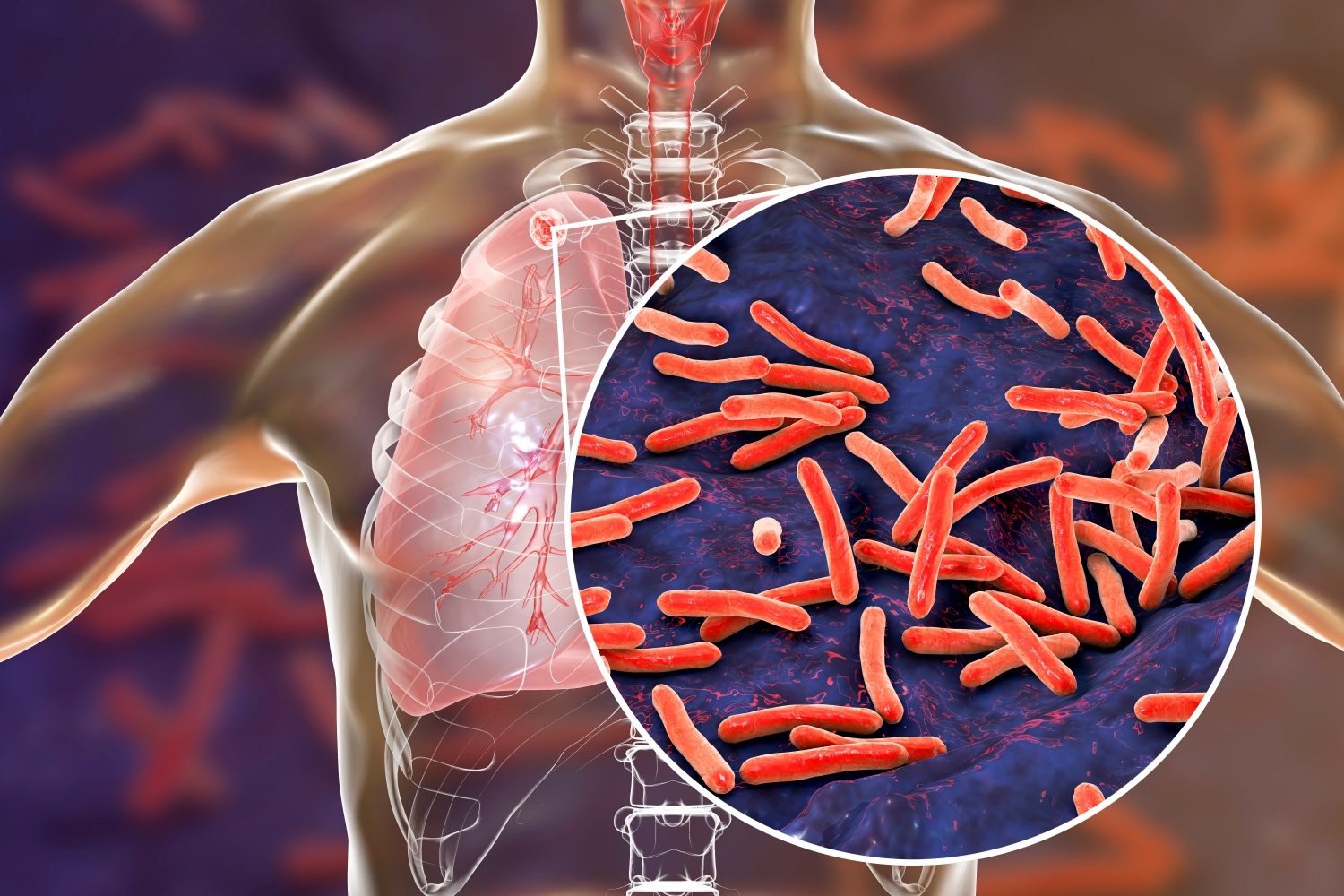
Bringing Taiwan’s MDR-TB Treatment Experience to the World
Dr. Chen-Yuan Chiang’s original interest lay in psychiatry. But as he ran into difficulties reconciling Western theories with an Eastern culture, he decided to move to a combination of internal medicine and public health. After graduating from Kaohsiung Medical University, he went on to receive a Master of Public Health at the University of California, Berkeley in 2003, and a Doctor Philosophiae at the University of Bergen, Norway in 2012.
Now Dr. Chiang spends about half of his time in Taiwan and half globetrotting as a national level advisor for tuberculosis related public health programs through The Union, where he has been working since 2003 when he was invited to join for his expertise in TB and lung disease. In this capacity Dr. Chiang often operates at the national policy-making level, being invited by governments and national or country level advisors to provide guidance on public health program implementation.
In 2007 Dr. Chiang was invited to establish a department of lung health and non-communicable disease in The Union. Through this department he implemented pilot projects to deal with the management, diagnosis, and care of patients living with asthma in mainland China, Sudan, Benin, and El Salvador. Although effective asthma treatments do exist, patients in resource-limited settings may not have access to care, while asthma medicines that are available may not be affordable or quality assured.
Management of MDR-TB: A Holistic Approach
Treatment success for TB in mainland China sat around 50% under the global fund project. However, increasing out of pocket expenses seems to have been a major barrier in MDR-TB treatment. With a CAP-TB project seeking to address the challenge in the management of MDR-TB, Dr. Chiang was invited to look into the components of treatment processes as a technical adviser to determine how best to make a positive impact on patient care.
The CAP-TB project takes a holistic approach that looks beyond physical symptoms to include patients’ family and life situations. In addition to out of pocket expenses for treatment that can mean injections and oral medications every day for 18 months, the burden of indirect costs, such as for transportation to a distant clinic, can prevent patients from completing treatment. For example, a 9-month MDR-TB regimen pilot project in the Philippines showed a promising increase in treatment success. However, the proportion of patients lost at follow-up remained substantial. According to Dr. Chiang, many MDR-TB patients end up stopping treatment or taking medications irregularly, not because of side effects or adverse reactions, but “most of the time the supporting system wasn’t good enough. You can imagine, the patients they are young, they may have babies… and need to travel every day to the facility for injections and oral medicine, it doesn’t work. It means that you need to take the patient’s perspective to understand the difficulty.”
These problems are what the CAP-TB project in Yunnan and the TREAT TB programme in the Philippines try to address. Thanks to Dr. Chiang’s input, the Cap-TB project includes a patient centered support group that leverages mobile phones and the internet to provide a support services package including regular meetings with patients, a 24-hour hotline, treatment reminder calls from nurses, and even help for patients to physically get to treatment. The project aims to build a sense of community and group belonging that can support patients emotionally as well as physically, with the end goal of better treatment outcomes. In the Philippines, the TREAT TB programme took the advice of Dr. Chiang to focus on treatment interruption and to decentralize treatment services to the community.
Although it’s still early to show treatment results, Dr. Chiang was informed that Yunnan’s MDR-TB treatment program is the most successful in mainland China. “They sent an email to me to say ‘We are so proud, so happy!’ But there’s still room for improvement. A success rate approaching 60% isn’t good enough.” Dr. Chiang would like to see a number closer to 80%, one that he thinks would be possible through a shortened but effective 9-month treatment regimen.
Policy-making from the Streets
The project in Yunnan is one of many that Dr. Chiang is involved with around the world. He makes regular advisory visits to Mongolia, Nepal, Vietnam, Sudan, the Philippines, Papua New Guinea, Thailand, and Laos. And his trips to Vietnam are set to increase. Just this year a Taiwan-Vietnam project has been initiated through TMU with funding from the Taiwan CDC, so more trips are planned to help bring a holistic approach to MDR-TB treatment and care to Quảng Ninh province in Vietnam.
Although much of his time is spend in policy discussion, Dr. Chiang still finds time to visit those in the trenches, where his interest in psychology comes in handy with patients who approach a doctor not necessarily for lung disease, but for cardiac symptoms, stress, or even emotional reasons. “You can understand [the patients] and know their complaints… You don’t take them just like an organ, you approach them as a human being. It’s quite useful”
Speaking with local clinicians is also valuable to someone with unique experience both as a clinician and in public policy. Whenever possible, Dr. Chiang takes a day out of each trip to understand doctors’ impressions of how the programs created in international meeting rooms are actually implemented. “It doesn’t matter what your policy says, if you cannot provide services properly then those things on paper will not work.”
Back in Taiwan
Dr. Chiang still enjoys speaking with students, so he finds time to discuss cases with them when he’s back at Wanfang Hospital. Students today have the freedom – and challenges – of choosing between a wide range of career paths, and they have increasing opportunities to develop an international perspective through travel. “It’s important for them to be well trained and be a master of medicine or surgery or the field they are interested in. They need to really enjoy what they are doing and develop their interests. It’s important for them to see the whole spectrum of what’s possible.”
1. Nunn, A. J., Phillips, P. P. J., Meredith, S. K., Chiang, C. Y., Conradie, F., Dalai, D., … Rusen, I. D. (2019). A trial of a shorter regimen for rifampin-resistant tuberculosis. New England Journal of Medicine, 380(13), 1201-1213. https://doi.org/10.1056/NEJMoa1811867
Dr. Chen-Yuan Chiang
Associate Professor, Division of Thoracic Medicine
Research Center of Thoracic Medicine-TB, Taipei Municipal Wanfang Hospital
Read more about his research
For interviews or a copy of the paper, contact Office of Global Engagement via global.initiatives@tmu.edu.tw.